Click to Skip Ahead
Dental care for your cat is as important as dental care for yourself. Cats can get tartar, gingivitis, broken teeth, tooth root abscesses, and dental pain just like us. The difference is that you cannot tell your cat to go and brush their teeth. You alone are in charge of monitoring and taking care of your cat’s dental health. Many cats will end up needing a dental cleaning at least once, if not multiple times, in their life.
Many people are surprised to learn that anesthesia is needed for teeth cleaning in our beloved pets. While anesthesia may sound scary, it’s actually the safest way to appropriately clean your cats’ teeth due to the nature of the cleaning and the stress that dental cleanings can cause for cats. Keep reading to find out more.
Dental Disease and the Importance of Teeth Cleaning
Dental disease in cats can appear in a myriad of ways. One of the most common things we will hear from owners is that their cat has bad breath. While this can definitely be a sign of dental disease, it doesn’t always mean your cat needs a dental cleaning. Many cats eat food that has fish in it. This may cause an odor to your cat’s breath that is noticeable, whether or not they have dental disease. However, halitosis, or chronic bad breath, can definitely be a sign of dental disease.
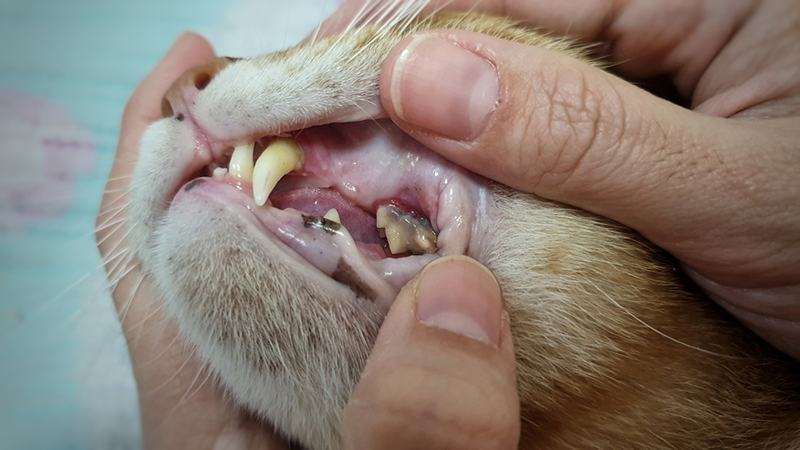
Other times your veterinarian may notice visible tartar on your cat’s teeth, or gingivitis along the gumline. Gingivitis will appear as reddened or dark pink gum tissue right along the gums where it meets the teeth. Sometimes evaluating all of the teeth is not possible – would you stick your hand into a strange cat’s mouth if they were nervous? But your veterinarian should get a good idea of dental disease by looking at the teeth your cat will allow them to see.
Why Does My Cat Need Anesthesia for Teeth Cleaning?
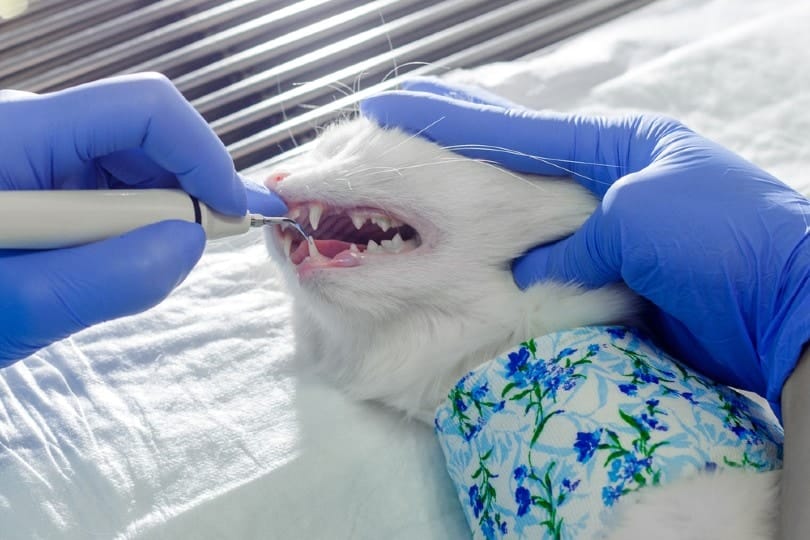
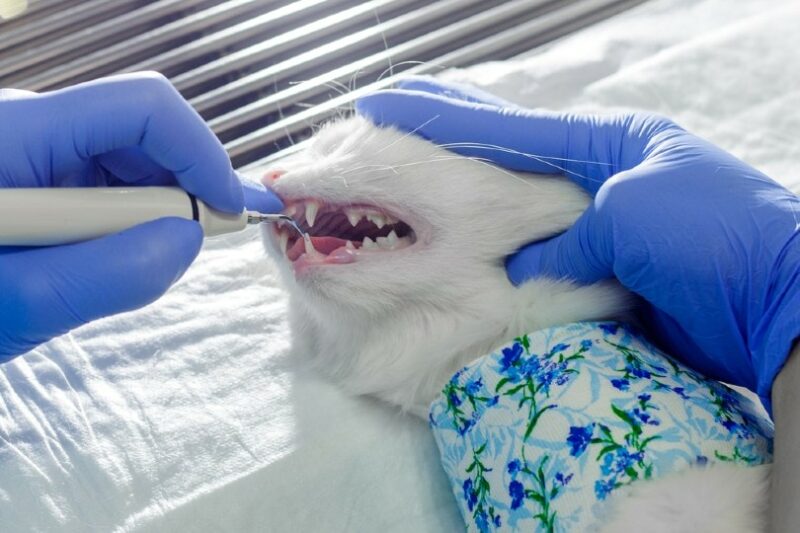
Anesthesia is actually the safest way for your cat to have a thorough, effective, full dental cleaning. Think about when you go to the dentist – how many times do you have to turn your head, open or close your mouth, spit, or move the slightest bit so that your dentist can do their job? Now imagine trying to do that in any awake cat. No matter how well behaved your cat is, having an assistant hold their mouth open, forcing instruments in to clean their teeth and doing an effective job just won’t happen. Not to mention the stress it will cause your cat.
When anesthetized, your cat sees, feels, and hears nothing. They are completely without stress of the situation and what is going on. This allows your veterinarian and their technician to thoroughly look at the entire mouth – not just a few teeth – take radiographs, clean all visible tartar, and use delicate instruments to clean the bacteria and tartar underneath the gum line. While anesthetized, any broken or diseased teeth can be safely removed, and their mouth can be evaluated for any abnormalities such as tumors.
In addition, the tube that is placed into your cat’s trachea to help them with breathing and anesthesia is actually protective. It not only allows appropriate oxygen and carbon dioxide exchange during the procedure, but it also protects any tartar, water, fluid, and bacteria from being sprayed and inhaled into your cat’s airways and lungs. If your cat didn’t have that protection of their airway, all of that bad material being removed from your cat’s teeth would be free to set up shop in their trachea and lungs, potentially causing pneumonia or other serious side effects.
What Happens During Anesthesia?
If your veterinarian recommends that your cat has a dental cleaning, it’s always recommended to do a physical exam and bloodwork within a few days to weeks of the procedure. Your veterinarian wants to make sure that your cat’s heart sounds normal (no obvious murmur or arrhythmia), is breathing normal, and has normal organ function on bloodwork. This will help to ensure that your cat is the best possible candidate to receive anesthesia and properly metabolize the drugs that are given.
On the day of the dental, your cat will likely have a pre-medication to help calm them down. This is typically given into the muscle or under the skin. An IV catheter is then placed so your cat can receive more medications to help them fall asleep. Once asleep, the tube is placed into their trachea to both help them breathe, and safely administer anesthetic gas and oxygen.
Your veterinarian and their technician will hook your cat up to machines that constantly read their heart rate, heart rhythm, blood pressure, oxygen levels, and body temperature. This helps them adjust anesthetic protocols or even stop if there are complications. Once the procedure is finished, your cat is slowly recovered and may even have some injections for antibiotic and pain coverage, depending on what has been done.

What Else Can Be Done Besides Anesthesia?
Preventive and routine dental care is always recommended for our feline patients. Doing this regularly may help prevent any anesthetic dental procedures from having to be completed. At minimum, it’s better for your cat’s long term oral and complete body health.
Teeth Brushing
The best thing for preventative, routine dental care is brushing your cat’s teeth. Always use toothpaste made specifically for pets – never use human toothpaste! Pet toothpaste is specially formulated to be safe to swallow in small amounts. It’s also flavored for our pets. Human toothpaste can be toxic, so please heed this warning and don’t use it. You can use a small baby toothbrush or a finger brush to gently scrub your cat’s teeth a few times a month. If your cat won’t allow the act of brushing, but likes the toothpaste, even rubbing a small amount over the surface of the teeth will help.

Prescription Food
There is also prescription “dental food” nowadays that acts similarly to brushing teeth. This food can be given as treats, or just mixed into your cat’s regular food to help scrub their teeth and keep them clean. The food is formulated with specific ingredients and enzymes for dental and gum health. You’ll need to get this through your veterinarian. The cost may sound expensive but keep in mind that you are only using a small amount weekly – typically this food does not replace your cat’s regular diet. Therefore, a small bag will last a very long time.
Dental Treats
There are a few dental treats that may help but know that they are not all created equal. This is a list of products that are recommended and approved by the Veterinary Oral Health Council (VOHC). These are the only products that most veterinarians will recommend and have been proven safe and effective. Other products ordered online may have a bunch of flashy, eye-catching marketing, but otherwise be completely useless. Know that by the time you spend a bunch of money on junk from the internet with flashy ads, you could’ve purchased a recommended and effective product from the VOHC list.

Conclusion
Dental health and routine dental care are extremely important to our feline patients. Dental disease does not only occur in people but affects many of our beloved feline companions as well, causing bad breath, tartar, pain, and infection. While routine dental care is always recommended, an anesthetic dental cleaning may be needed. Anesthesia is actually the safest recommended procedure for your cat so that they not only stay stress free, but can have a complete and thorough exam and cleaning.
Speak to your veterinarian about their pre-anesthetic requirements and their specific anesthetic protocols. Never trust a veterinarian who says they can clean your cat’s teeth just as well without anesthesia. In the end, anesthesia keeps your cat safe, stress-free, and allows them to get the best standard of care.
Featured Image Credit: Burdun Iliya, Shutterstock