Click to Skip Ahead
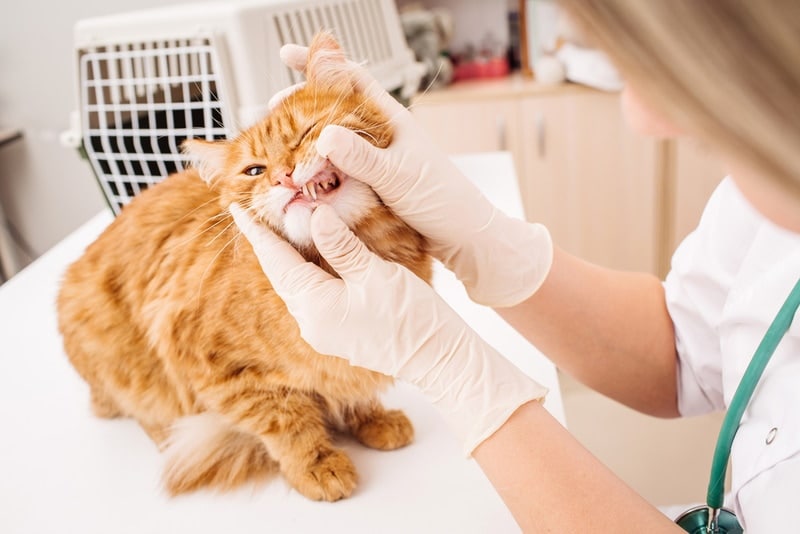
Did you know that February is Pet Dental Health Month? It’s true, and though this facet of our pet’s care is often forgotten about, it is very essential. Just as with humans, your cat’s dental health can affect their entire well-being, so creating good dental habits early is critical.
If you believe your kitty is suffering from toothache or dental pain, you’re probably wondering what to expect when you take them to the vet. What could be causing their pain? What signs should you be on the lookout for? We’re here today to answer these questions, so read on to learn everything you need to know about cat toothache and dental pain, including what to expect as far as treatment for some of the more common conditions.
What Is Cat Toothache Pain?
In a perfect world, our cats could look us in the eye and tell us that they’re having tooth pain. In the real world, this isn’t possible.
Dental issues can have severe consequences if not addressed and treated properly. Dental diseases can cause extreme pain and discomfort, impacting a cat’s quality of life. A cat with a toothache may be uninterested in eating, affecting their energy level and mood. Additionally, when a cat doesn’t eat for as little as 24 to 36 hours, they may be at risk of developing a life-threatening condition known as hepatic lipidosis. So, it’s not just your cat’s oral health at risk here.
The good news is that many common dental conditions affecting cats are preventable or treatable with appropriate precautions and monitoring.

What Are the Signs of Cat Toothache Pain?
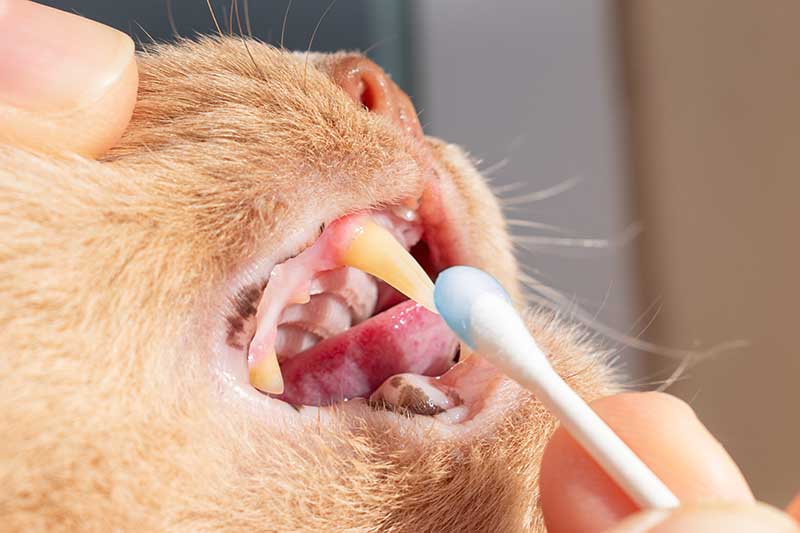
Unfortunately, dental pain can take on many appearances depending on the severity, cause, and your pet’s personality. Since cats are experts at hiding pain, they may not show any signs of hurting at all. Some owners don’t even realize their pets are in pain until a veterinary exam indicates otherwise.
However, you may sometimes observe signs of toothache pain at home. The most common signs include:
- Bad breath
- Bleeding gums
- Chewing slower than usual
- Decreased interest in eating kibble or treats
- Dropping food
- Excessive drooling
- Head shaking
- Pawing at the mouth or head
- Reluctance to groom
- Swallowing dry food whole
- Swollen gums
- Vomiting
- Weight loss
What Are the Causes of Cat Toothache Pain?
According to the Cornell Feline Health Center, the most common causes of cat toothache or dental pain in cats are gingivitis, periodontitis, and tooth resorption. However, cats can also develop stomatitis, malocclusions, or oral tumors. Each condition can vary in severity, so the sooner you’re able to catch and treat them, the better the prognosis (and the less pain your pet will be in).
Gingivitis
Gingivitis is a gum-related condition noted by inflammation. The process generally begins when a thin layer of bacteria-containing plaque builds up on the teeth. If this is not removed, it can migrate deeper toward your cat’s gumline, causing an immune system response and inflammation. Gingivitis can be reversible, though the treatment will depend entirely on how severe it is.
Periodontitis
Periodontitis can develop if gingivitis is not treated promptly. Unlike gingivitis, this condition may not be reversible if it progresses to a certain point. Periodontitis is marked by severe tissue damage. It affects the gums, ligaments, and underlying bone. It can cause loose teeth and even tooth loss.
Tooth Resorption
Cats don’t develop cavities like humans; instead, they develop resorptive lesions. Tooth resorption involves the breakdown of the entire tooth structure. It begins inside the tooth and can often progress to other parts. This is the most common cause of feline tooth loss and can be extremely painful.

Stomatitis
Stomatitis is a painful and complex oral condition with marked inflammation. It may develop in cats having an adverse reaction to their own plaque and mouth bacteria. It is marked by a generalized inflammation of the mouth’s mucous membranes and may also involve the lip surfaces, and back of the mouth, and gums.
Malocclusions
Malocclusion refers to an abnormal tooth alignment that can be either skeletal or dental. Skeletal malocclusions occur when there’s a discrepancy between the lower jaw and upper lengths. It causes affected cats’ teeth to be out of normal orientation. Dental malocclusions happen when one or more teeth are out of alignment.
Oral Tumors
According to Cornell University Hospital, oral cavity cancer is the fourth most commonly diagnosed cancer in cats. It accounts for 15% to 20% of feline malignancies seen at this hospital. As with other types of tumors, some will grow slowly and not spread (benign), while others will be aggressive and spread rapidly (malignant). Unfortunately for our feline friends, more than 90% of oral tumors are considered malignant.
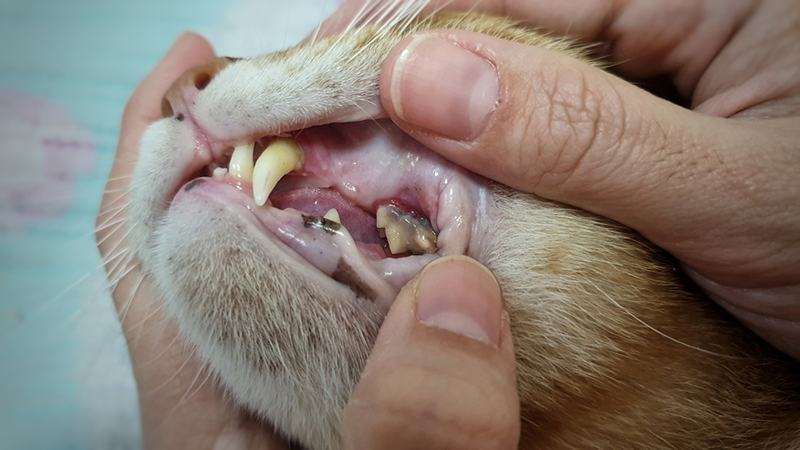
How Do I Care for a Cat With Toothache Pain?
The care required for a cat suffering from tooth pain will depend on the root cause of said pain. In most cases, you’ll be working closely alongside your veterinarian.
Gingivitis
If gingivitis is the cause of your cat’s dental pain, their treatment plan will depend on the severity. You can expect to be encouraged to brush their teeth, and your vet may recommend antibiotics in pill form or as an oral rinse. They may also suggest tooth scaling or removal if that is the only way to remove the inflammation.
Periodontitis
If your pet’s gingivitis has progressed into periodontitis, your vet will likely recommend a thorough cleaning done under anesthesia. They’ll take X-rays during the cleaning to determine how much bone was lost and if any teeth need to be removed.
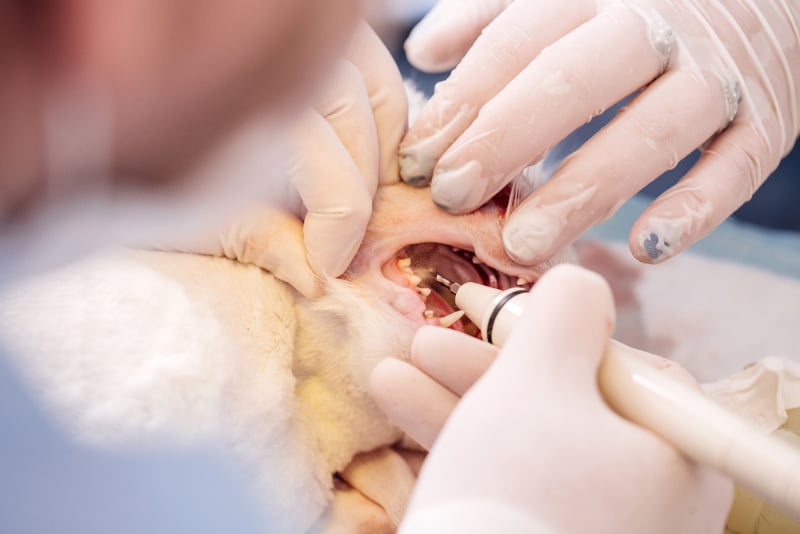
Tooth Resorption
If your cat has been diagnosed with tooth resorption, your veterinarian should focus on managing their pain and preventing the condition from progressing. Some teeth will need careful monitoring, while others may need to be removed altogether.
Stomatitis
Your vet will need to treat the underlying cause of stomatitis if one can be identified. Unfortunately, it is very common for no specific cause to be found. Cats with this condition may need frequent dental cleanings and extractions; potentially even all their teeth may need to be removed. Your vet may also prescribe pain medications, antibiotics, or anti-inflammatories.
Malocclusion
Treatment options for malocclusion will depend on the cause and severity. It may include extractions of the offending teeth.
Oral Tumors
Surgical removal of the tumor is the standard treatment if possible.. In some cases, surgery is not an option. In these cases, radiation therapy can be tried, though success rates are not great. Euthanasia is commonly recommended.
Frequently Asked Questions
Why does veterinary dentistry require anesthesia?
We get it; going to the vet is expensive, and having to pay for anesthesia to have your cat’s dental issues treated or diagnosed can be a huge hit to the ol’ budget. However, there are good reasons why veterinary dentistry requires anesthesia.
When you go to the dentist, your doctor expects you to sit still and can talk to you about your pain levels and discomfort. The same cannot happen when your cat goes to the dentist. Your cat doesn’t understand why their mouth is being forced open and will often react by trying to escape or even becoming aggressive. Anesthesia then is required not only to keep your cat still and calm and make for easier diagnosing and treatment but also to protect the veterinarian providing their care. X-rays also cannot be done in pets unless they have been anesthetized.
What can I do to promote oral health at home?
Prevention of common feline oral diseases requires frequent plaque and tartar removal. Regularly brushing your cat’s teeth is the most effective thing you can do to promote oral health at home. As you can imagine, cats can be pretty resistant to the idea of brushing, but with some patience, training, and lots of yummy rewards, it can be done.
Conclusion
Oral health is just as important for our cats as it is for us. Toothaches and other similar dental conditions can be extremely debilitating and even life-threatening in some situations, so keep on top of your cat’s oral health. Frequent preventative teeth cleanings and annual wellness exams at the vet will go a long way in preventing some of the dental issues your cat may face. Additionally, you can do your part at home by committing to brushing your teeth as often as they’ll let you.
Featured Image Credit: PRESSLAB, Shutterstock