We all want the best for our pets. Sometimes, they make it challenging, as cats are well-known for their penchant to hide illnesses and injuries. It’s the wild feline in them, reminding them not to appear vulnerable. However, observing your kitty can tell you a lot about how they feel, both physically and mentally.
Fortunately, many non-invasive strategies can give you a head-up about your cat’s health. Listed below are 12 ways to ensure that your cat is healthy without leaving the comfort of your own home.
The 12 Signs of a Healthy Cat
1. Their Presence
The mere presence—or absence—of your pet tells you a lot about their state of health. A sick or injured cat often hides, sometimes in unusual places, as it provides comfort and stress relief, which are needed when a kitty isn’t feeling their best. While a cat hiding from time to time is not unusual, excessive hiding is definitely a red flag.

2. Activity Levels
A cat that feels well remains active, although the patterns may vary with the individual animal. Is your cat still playful? Do they get the zoomies a couple of times a day? Are they interested in games and puzzle feeders? If yes, then these are all signs of a healthy kitty.
3. Appetite
Your cat’s appetite is an excellent health indicator. While sometimes finicky, most felines are food-motivated. Keep in mind that it can be difficult to tell how much your pet is eating if you free-feed them, so we recommend setting specific mealtimes so that you can observe their behavior and overall food intake. If they’re excited about dinner and all seems normal, your cat is likely in good health.

4. Sleep Schedule
Sleep is vital for you and your cat. Our pets are pros, with adults snoozing roughly 16 hours daily. However, excessive sleeping may be a sign that something’s wrong.
5. Litter Box Habits
A cat’s litter box habits can tell you a lot about what’s going on under the hood. It can point to things like GI issues or urinary tract problems if your pet is missing the box or straining. While not diagnostic, GI distress can point to accidental ingestion of something poisonous, food intolerances, or other health problems. Urinary tract issues can have a wide variety of causes including urinary stones, infection and stress. Whenever your cat’s litter box habits aren’t normal, take this very seriously and get them checked out by a vet as soon as possible.

6. Coat Appearance
Many cats are fastidious self-groomers. They may spend up to half their waking hours taking care of themselves. A healthy kitty has a shiny, neat appearance, particularly if you feed your pet a good diet. A rough coat or bare patches can indicate nutritional deficiencies, or it can signal an allergy, behavior problem, or external parasites. We suggest scheduling a vet exam to determine the cause if your cat’s coat isn’t well-groomed and healthy-looking.
7. Body Condition
Your kitty’s body condition can reveal your pet’s weight status, whether overweight or underweight. The former may require a diet change and close monitoring, and the latter requires veterinary intervention to figure out the cause, especially in cases of unexplained weight loss. It can have relatively easily managed conditions, such as internal parasites, but it could also mean something more serious.

8. Mobility
Cats are remarkably mobile and agile animals. Undoubtedly, you’ve witnessed your kitty tearing around the house in a sudden burst of energy to work off some steam. That’s a sign of a healthy, content pet. But you should also pay attention to your cat’s gait for any signs of limping or pain. These animals have an excellent talent for landing correctly. However, joint conditions, like arthritis, can affect their mobility and overall health.
9. Body Language
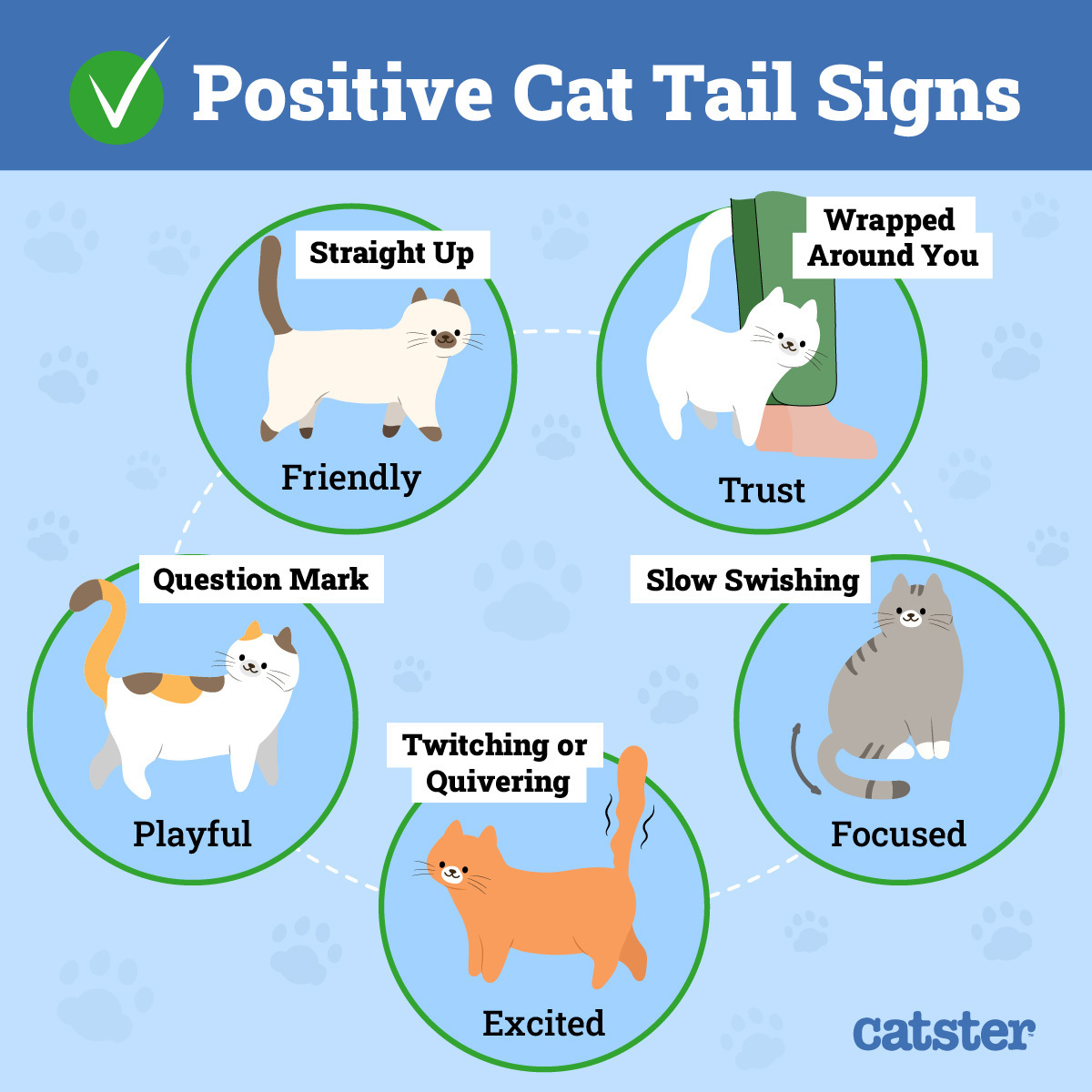
Cats may like to hide, but their body language makes them an open book. Their tail and ear positions reveal much of what they’re feeling. For example, if they hold their tail upright, all is well. Likewise, keeping it low to the ground may mean your kitty is in pain. Feline body language is also a form of silent communication. An irritated pet will warn others by tapping their tail before things escalate. If you are able to recognize the signs of an unhappy pet, this would be a good indicator that they need to be seen by a vet for a check-up.
10. Eye, Ear, and Oral Health
A quick glance at your pet can often give you a good idea of how they’re feeling. For example, their eyes should be bright, clear, and free of discharge. Their ears should be clean and free of discharge, redness, or odors.
Unfortunately, our pets usually need our help when it comes to dental hygiene. Ideally, you should brush your cat’s teeth daily. However, dental treats or a diet formulated for this purpose can help. Signs of a healthy mouth include a fresh smell, pink gums, and teeth free from plaque and tartar. You should also check them regularly for any sores or growths. However, if all is well in the mouth area, then your kitty might be pretty healthy too.
11. Mental Well-Being
Your pet’s mental well-being is an excellent indication of their overall health. A cat without adequate enrichment will likely engage in unwanted behavior, such as scratching, inappropriate elimination, or destruction. Sometimes, they will do things to get your attention, whether good or bad. We encourage you to provide your kitty with scratching posts and interactive toys to challenge them mentally, thus leading to a healthier life for your cat.

12. Social Interactions
A sick or injured cat is less likely to interact with family members. Instead, they may hiss or growl to fend off any attempts. A feline may also be cranky if they’re sleepy. A healthy, happy kitty won’t shun social interactions if properly socialized. So, sudden changes in behavior might suggest something hurts and needs investigating.
Tips for Keeping Your Cat Healthy
Giving your pet a food formulated for their life stage is essential for your cat’s good health. It will ensure they’re receiving adequate nutritional support. We recommend monitoring your kitty’s body condition and adjusting their diet as necessary to maintain a normal weight, as obesity increases their risk of chronic health conditions, such as diabetes.
We recommend annual exams for your cat at a minimum. That will ensure they’re up to date on vaccinations and routine tests. Sometimes, the latter can detect the early stages of a condition and improve your pet’s prognosis if your vet diagnoses something. Remember that felines hide health problems until they can’t keep up the ruse any longer.
Keeping your cat indoors is often the safest and healthiest option for them. Indoor cats are at lower risk of contagious diseases and parasites, they are also not exposed to outside dangers like traffic or other animals. However, you must ensure an enriched indoor environment so cats are able to express their natural behaviors, including scratching and playing.
Conclusion
As much as cats like to hide, they can’t conceal everything from us if we pay attention to their behavior and appearance. It’s helpful to know the good and bad signs to help you provide the best care for your pet. That will empower you to make good choices for your feline companion and ensure a long, healthy life for years to come.
Featured Image Credit: Vershinin89; Shutterstock













