Click to Skip Ahead
We all want to provide our cats with the best possible care, and for many of us, that means following the most modern and up-to-date information and technology. However, more and more people are looking for alternative ways to optimize their pet’s health—as well as their own—using more natural methods and a holistic approach. But what does that really mean?
For many of us, the phrase “holistic therapy” conjures up images of healing crystals, meditation, and herbal medicine, but this is merely a tiny fragment of what holistic therapy really means. In fact, many would argue that it is something that every doctor, therapist, or clinician should be aiming for because a holistic approach, by its very definition, means to treat a problem by addressing the whole patient, not just the symptom in front of you.
Let’s take a closer look at what holistic care for cats is and how it can benefit your feline friend.

What Is Holistic Therapy?
Holistic therapy is an approach to treating a patient that looks at the problem, symptom, or complaint in terms of how it relates to or is affected by the body, lifestyle, habits, mental health, and emotional well-being. It incorporates standard medical techniques and treatments alongside more traditional and natural cat care methods, such as traditional Chinese medicine, including acupuncture, herbal supplements, environmental factors, and diet, to create a more personalized treatment plan.

An Example of Holistic Therapy
Quincy is 12 years old and has been mildly lethargic, has not been eating well for almost a month, and has been spending a lot of time curled up in the spare room upstairs. He is drinking and toileting normally.
A symptom-based approach finds nothing terribly remarkable on his physical exam. He has actually put on a little bit of weight but looks thinner over his hindquarters and is a bit stiff on his back legs.
The vet runs some blood tests and finds nothing abnormal with his kidneys, liver, or thyroid, and his blood sugar is normal. He is prescribed some pain relief for suspected arthritis, with instructions to report back for a recheck after a week.
The holistic approach finds all the same things as the symptom-based approach and runs the same blood tests but also learns that the owner’s child has just started walking, and Quincy has been avoiding the baby, although he is often found in the dining room after the baby has finished dinner and is having a bath. Since the baby started walking, the parents had to remove Quincy’s cat tree as their baby nearly pulled it over.
- Some pain relief medication for suspected arthritis, with a plan to come back in a few days to start acupuncture
- Pheromone plug-in diffusers to help alleviate Quincy’s stress now that the baby is more mobile, which could be causing some anxiety for him
- Replace Quincy’s cat tree with a more sturdy substitute so he has somewhere he can safely retreat to when needed
- Clear up any food scraps left over from the baby’s dinner – it is likely that Quincy has been helping himself!
Although a symptom-based approach isn’t wrong, it is less likely to address the whole problem and is therefore less likely to result in a long-term solution. Of course, a holistic diagnostic and treatment plan is much more time-consuming, which can often limit our ability to put it into practice.

What Holistic Therapy Is Not
- A replacement for veterinary treatment/care. It should incorporate both modern medicine and natural alternatives; it should not be one or the other.
- Homeopathy, or the use of heavily diluted substances to treat a range of ailments. It has been widely rejected by both the scientific community and practitioners of reputable natural therapies as being ineffective at best and dangerous at worst.

Holistic vs. Symptom-Based Approach
| Holistic | Symptom-based | |
| Pros |
|
|
| Cons |
|
|
Let’s explore some ways that you can work together with your vet to treat your kitty in a healthy, holistic way.

Holistic Cat Care: 8 Natural Ways to Keep Your Kitty Healthy
Although not exhaustive, the following list shows us how we can take a holistic approach to our cat’s health and wellbeing.
1. Diet

One of the simplest ways to improve your cat’s health is by making sure you are providing them with a diet that is right for them. It is now easier than ever to source high-quality, pre-prepared fresh food for your cat that is free from grains, additives, and preservatives, and you can even have it delivered to your door. It is important to remember that what is an ideal diet for one cat may not be suitable for another, so making sure that you are selecting a food that is right for your cat’s age, weight, activity level, and health concerns is vital.
2. Feline Feng Shui
Take a walk around your home and try to look at it from your cat’s perspective. Are there places to jump, climb, hide, and sleep? Can they get away from noise and activity when they need to? Are their beds, food, water bowl, and litter box in places that are quiet and away from foot traffic? Sometimes, when we make our homes more child-safe or Instagram-worthy, they become less cat-friendly, so it’s a good idea to stop every now and then and get a “cat’s-eye view” of their environment.
3. Acupuncture, Acupressure, and Massage
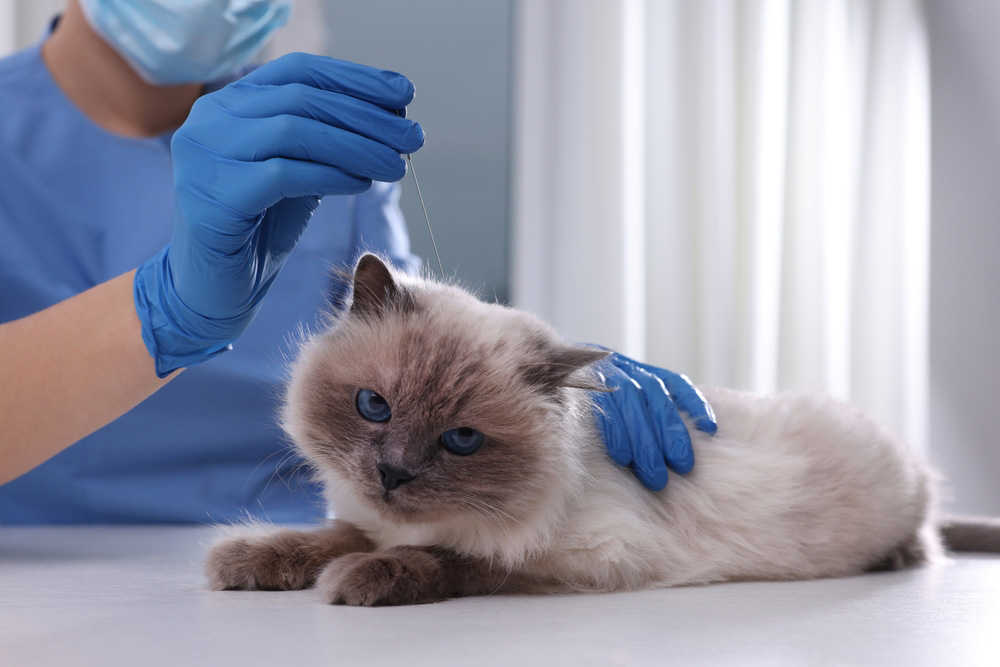
Whether your cat suffers from arthritis or just occasional aches and pains, there are a number of ways you can help improve their comfort without relying solely on drugs. Acupuncture is increasingly used in veterinary practice and can help treat a wide range of health problems, including arthritis, asthma, IBD, and even stress. Acupressure uses similar points to those used in acupuncture but without the use of needles, so it is something you can do at home. Massage is a great way to treat your cat and improve your bond.
4. Supplements
Herbal remedies and supplements can be extremely beneficial for your cat and can help improve joints, stress, IBD, urinary tract health, and skin and coat conditions. Be very careful about what sort of supplements you use, as not all herbal remedies are safe for cats. The best option is to check with your vet before starting your cat on any supplements to make sure they are safe for your kitty and that you’re not about to waste your money.
5. Vaccination Customization

Vaccination can be a contentious issue for practitioners of natural medicine, but this is where compromise and collaboration are essential. The fact is, there are a number of diseases that our cats can be exposed to, some of which are deadly, others merely cause chronic illness. However, depending on your geographical location and your cat’s lifestyle, you may choose to vaccinate less frequently or only against certain viruses.
Communication with your vet is key, but it is possible to strike a balance between minimizing the risks of vaccination (which are very low) and protecting your cat from infectious diseases. It is important to be aware that any deviation from the manufacturer guidelines means that the vaccine efficacy will not be guaranteed.
6. Environmental Enrichment
Similar to the lines of our feline feng shui, this is about providing our cats with places to safely jump, explore, and enjoy their indoor environment, as well as giving them plenty of our time and attention. Having a rotating system of interesting toys is a great way to provide novelty without having to buy new ones every month.
7. Something in the Air

If you have multiple pets or young children, if the world outside (or inside!) your house is busy and loud, or if you are making some changes, renovating, or moving house, all these things can upset the serenity of your cat’s home. Some cats don’t show obvious signs of stress, but you might notice that they keep to themselves, like to hide under beds or in cupboards, only venture out after bedtime, or perhaps they’ve started to go to poop or pee outside their litter box—these can be signs that all is not well with your cat’s emotional health.
A veterinary exam should always be first on the list to make sure there are no physical problems, but introducing some pheromone or calming support into the air by using diffusers or sprays can work wonders on feline mental health.
Always select products that are designed with cats in mind, as many of the essential oils used to alleviate stress in humans are actually toxic for cats. And never underestimate the pleasure-inducing power of some catnip!
8. Regular Check-Ups
They say that “prevention is better than cure,” and this is certainly true when it comes to your cat’s health. A check-up with the vet once or twice a year is one of the best things you can do for your cat in terms of making sure of the following:
- They are a healthy weight
- Their teeth are in good condition
- Their heart and lungs sound healthy
- They have no lumps or swellings inside their abdomen
Although preventive health sometimes includes giving medication, it can also mean that we avoid giving stronger medication or needing more invasive procedures later on.

Summing Up
The hallmark of treating animals and humans is to first do no harm, and in this way, there are many natural and alternative approaches to healthcare that are perfectly suitable for our pets, provided that they do not pose a risk of causing damage, or of preventing them from receiving more appropriate treatment. Those who view holistic treatment as an alternative to modern medicine are missing both the point and the potential benefits. Taking a holistic approach to our cat’s well-being ensures that we are addressing all their needs and exploring all options for their health.
Talk to your vet about how you can take a holistic approach to keep your cat happy, healthy, and safe.
Featured Image Credit: Ground Picture, Shutterstock