Click to Skip Ahead
Despite the widespread use of anesthesia in veterinary medicine, some cat owners may be unsure about the details surrounding anesthesia or even apprehensive of its use for their feline friend. In this article, we’ll discuss more about the use of anesthesia in cats, when it may be recommended, as well as potential risks and precautions associated with it.
Knowledge can help combat uncertainty or fear and allow a cat owner to be more aware, prepared, and empowered for their cat’s overall health.
How Does It Work?
What exactly is anesthesia? One way to define it is that it is a controlled medical event that, through anesthetic drugs, allows for a loss of physical sensation (including pain) as well as the ability to control the level of consciousness. Depending on the type of anesthesia used, different purposes can include the elimination of pain (analgesia), not moving (muscle relaxation), being unaware (temporary amnesia and potential loss of consciousness), or a combination of all of the above.
Anesthesia is needed for medical reasons, such as during a procedure or surgery. Furthermore, various anesthetics can be used in combinations to achieve the best effect for the patient and what is being done.
Generally, when in effect, anesthesia works by temporarily blocking sensory signals that travel to the brain. Different types of anesthesia and the wide variety of anesthetic drugs can all work and achieve this in various ways. In fact, doctors and scientists are not always aware of how all anesthetics work, but some types can prohibit pain by decreasing nerve cell activation via changing the neurotransmitters (chemical messengers that distribute messages from nerve cell to nerve cell) which are released.
Alternatively, other types may block the transmission of signals altogether by not allowing the ions to move as they typically would.

What Are the Different Types of Anesthesia?
In veterinary medicine, there are a few types of categories of anesthesia that can be used by themselves or even in combination together.
- General anesthesia (GA): Results in full unconsciousness by suppressing the central nervous system. This involves intubation with a specialized tube to keep an open airway and an anesthetic machine to allow for a continuation of anesthesia for a longer period of time. Assisted breathing can also be utilized. An example of when general anesthesia would be used would be for a spay surgical procedure.
- Sedation: Suppresses the central nervous system but not as much as in general anesthesia, and therefore does not result in full unconsciousness. Depending on what is needed, the dosing and type of drugs used can achieve various levels of sedation such as light, moderate, and heavy. Sedation is typically used for shorter periods of time than general anesthesia and some types are also reversible. Some examples where sedation may be useful include obtaining a skin biopsy or lab samples for an aggressive cat.
- Regional/local anesthesia: Can be used by itself or in addition to general anesthesia or sedation. The purpose is to block nerve impulses to a specific area. Examples could include when placing sutures for minor wound repair or in combination with general anesthesia or using nerve blocks to numb the area around a tooth for removal during a dental procedure.
Different types of anesthetic drugs can be classified into various categories in several different ways. One such way is to categorize them according to the different routes in which anesthesia can be given, such as:
- Inhalable anesthetics are drugs that are vaporized and given as a gas paired with oxygen. They can be delivered from either a mask or through an endotracheal tube. Examples include isoflurane or sevoflurane.
- Injectable anesthetics can be given into specific anatomical spaces, depending on the drug. These most commonly include the vein, muscle, and/or subcutaneous (between the skin and muscle) spaces. An example includes propofol given intravenously.
- Via the oral transmucosal route. Some medications via the mouth may be an option and can allow for rapid absorption, are painless, and are usually well tolerated. An example in cats is opioids with or without dexmedetomidine.
- Local anesthetics are given via injection or placed topically to block pain from nerves in a specific area. Examples are Lidocaine or Bupivacaine.
Where Is It Used?
Because in veterinary medicine we can’t communicate to our patients that we are not trying to harm them or to have them hold still or move a certain way, we may use anesthesia as a more frequent tool than in human medicine to help with the overall health of a cat. Essentially, anesthesia may be required if the veterinary team needs a pet to hold still and to temporarily eliminate pain.
Regarding anesthesia, different needs may require different types. Surgery, such as a spay or neuter, a dental procedure, internal organ sampling or repair, large mass removal, or severe wound repair requires general anesthesia. In addition, different types or levels of sedation may be needed for procedures such as minor wound repair, skin biopsies, grooming, or obtaining an exam and lab work samples in an aggressive cat.
In the event that the safety of the cat and/or team members involved in their care are at play, anesthesia is a helpful tool to allow for a better situation for all involved.
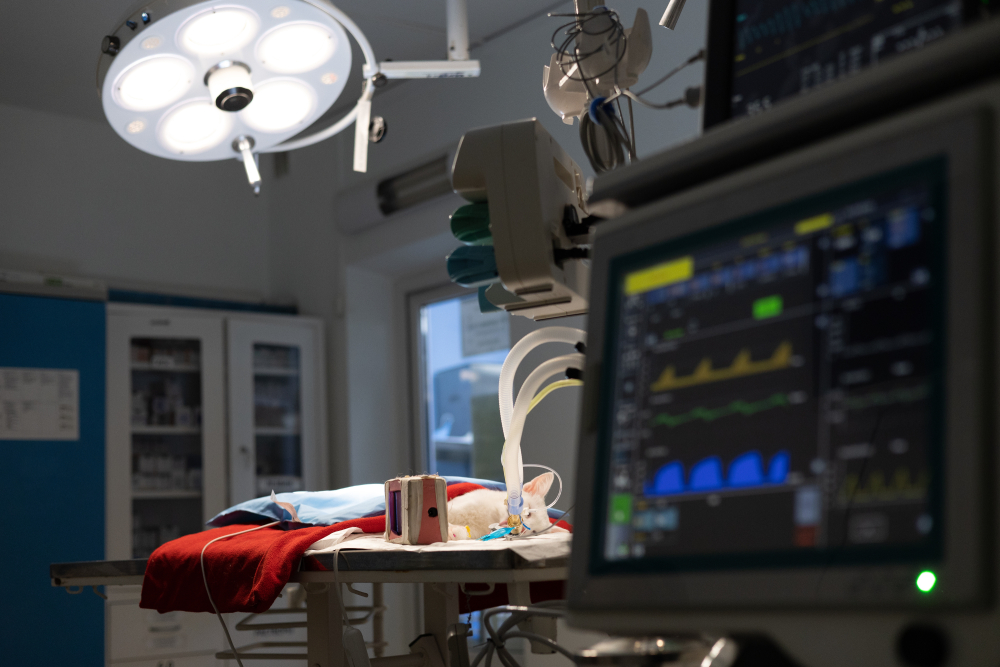
Risks and Precautions
Because anesthesia can bring on potential risk, or expose a cat to unique potential problems, taking special precautions or measures ahead of time to prevent something negative from occurring is very important.
Risks
Anesthetic risks can range from mild issues such as a small decrease in body temperature during the procedure or once awake or mild irritation due to the endotracheal tube placed in the airway, to more severe or life-threatening issues such as an anaphylactic reaction to the anesthetics or even the heart stopping (cardiac arrest) in reaction to the anesthesia.
A sampling of anesthetic risks during the procedure could include hypothermia (low body temperature), low blood pressure, irregular or abnormal heart rhythms, damage to the kidneys, etc. In addition, prior health problems or being in poor health, older age, variations from an ideal weight, and long procedures can also increase risk. While no procedure or need for anesthesia can be totally risk-free, veterinarians try to minimize the risk as much as possible.

Precautions
Some precautions that can be taken include a thorough history, a full physical exam, pre-anesthetic bloodwork, a catheter that allows for intravenous (IV) access, availability of emergency drugs, and having various anesthetic drug options that can best be tailored to different patients. In addition, checking the heart with a preoperative electrocardiogram (ECG) or other cardiac testing may be recommended.
Furthermore, if your veterinarian requests approval for specific tests or referral for further care prior to anesthesia, there are medical reasons for this, and those recommendations should be strongly considered.
Veterinarians and their teams often use many guidelines and checklists as well as intensive monitoring during (and even after) the anesthetic event to try to prevent or resolve problems in real-time. Monitoring includes trained personnel watching the pet dutifully during and after the procedure. Some components of observation include keeping an eye on parameters such as body temperature, breathing and heart rates, blood pressure, oxygen saturation (SpO2) and carbon dioxide levels, an ECG to monitor the heart, etc.
Risks vs Benefits
As the cat owner, considering the risks of anesthesia versus the benefits of the procedure is key. Some things you can do to help minimize your cat’s risk during anesthesia include having regular routine preventative care, ensuring your cat is at a healthy weight, and communicating all current medications/supplements and any past reactions from your cat to your veterinarian. In addition, following their pre- and post-anesthesia instructions is very important.

Cat Behavior After Anesthesia
After anesthesia, a cat will wake up while being monitored at the veterinary hospital, often for at least a few hours. Once they are awake and stable enough to be released to go home, it is important to note that they may not be quite themselves for a little while. Each cat will react differently to the effects of anesthesia.
Some cats may be more vocal, others more cuddly, some more aggressive, while the majority may want to be left alone as they readjust. At times, a cat may also have mild, short-lived gastrointestinal upset after the anesthesia such as mild nausea, not wanting to eat, vomiting, or changes in bowel movements. Overall, acting a little more disoriented, sleepy, and less active than normal for 12–24 hours after the procedure is fairly common.
If there are more severe or ongoing concerns, this should be brought to the attention of the veterinarian.
Frequently Asked Questions (FAQ)
What is a cat’s routine general anesthetic experience?
While each step is not set in stone, below is a common sequence of events that can occur for a cat receiving general anesthesia before a planned procedure, such as with a spay.
First, an accurate weight is obtained as well as a physical exam by the veterinarian. Next, any pre-anesthetic bloodwork or lab tests needed prior to anesthesia to determine an overall picture of their health are done. Placement of an intravenous (IV) catheter will allow for fluids during the procedure as well as for immediate drug access, including emergency ones should there be a need.
Once completed, evaluation of the bloodwork and lab tests will be used in conjunction with all other findings to help the veterinarian form a personalized anesthetic plan. Such a plan may consist of a combination of specific drugs from various classes that include a pre-anesthetic drug, intravenous induction drug, and anesthetic inhaled gas coupled with oxygen.
Just prior to the cat’s procedure time, the cat is given their anesthetic induction agent. Once that has taken enough of an effect, they are unaware of the placement of an endotracheal tube to allow for a clear airway. In addition, it will allow them to be hooked up to oxygen and the continued anesthetic gas which will keep them under anesthesia. Next, the placement of all monitoring equipment for the veterinary team to use as tools throughout the duration of the procedure will happen.
Once the procedure is complete, removal of the anesthetic gas and oxygen will prompt a cat to begin the waking up process and they will continue to be monitored closely by the veterinary team. Once confirmed to be awake and stable enough to be able to swallow, the endotracheal tube will be removed. Before going home, the IV catheter will be taken out and bandaged, and important discharge instructions with the cat owner will occur.
At several points in this process, communication with the cat’s owner may be necessary. For example, discussing significant bloodwork findings, or letting them know of any significant or problematic changes before, during, or after the procedure. In addition, it is common to receive a call to update a cat owner when their feline friend is waking up from anesthesia and to let them know how the procedure went.

Are certain breeds of cats more at risk under anesthesia?
Cat breeds that are brachycephalic (have a flat facial appearance), such as Persians and Himalayans, have unique facial and airway anatomy that can make them more at risk than non-brachycephalic cats. Veterinarians and their teams are aware of these risks and may tailor a brachycephalic cat’s anesthetic event a little differently to do their best to mitigate these differences.
Can my cat die under anesthesia?
Overall, anesthetic death is extremely uncommon, but it can occur. In one study that evaluated the death rate of anesthetic-related events in cats, it was quantified at 11 cats per 10,000 (0.11%) episodes of anesthesia. Some of the increase in risk was found to be related to aging cats, those not monitored with SpO2 or those with higher body weight. In another study, it was found to be about 1 in 900 anesthetic episodes. We don’t always have all the answers about why these events happen, even when infrequent.
Regardless, we attempt to have this number be as low as possible by utilizing precautions, putting as many safeguards into practice as possible, and continuing to learn and make changes with new information.
Conclusion
Having a cat undergo anesthesia can ultimately be beneficial for their overall health. Knowledge about anesthesia’s basics, uses, risks, and precautions can be valuable for the inquisitive cat owner. For those who still may have concerns or anxiety, a conversation with your veterinarian about the benefits versus risks as well as their clinic’s precautions and safety practices may also be helpful.
Featured Image Credit: KDdesign_photo_video, Shutterstock